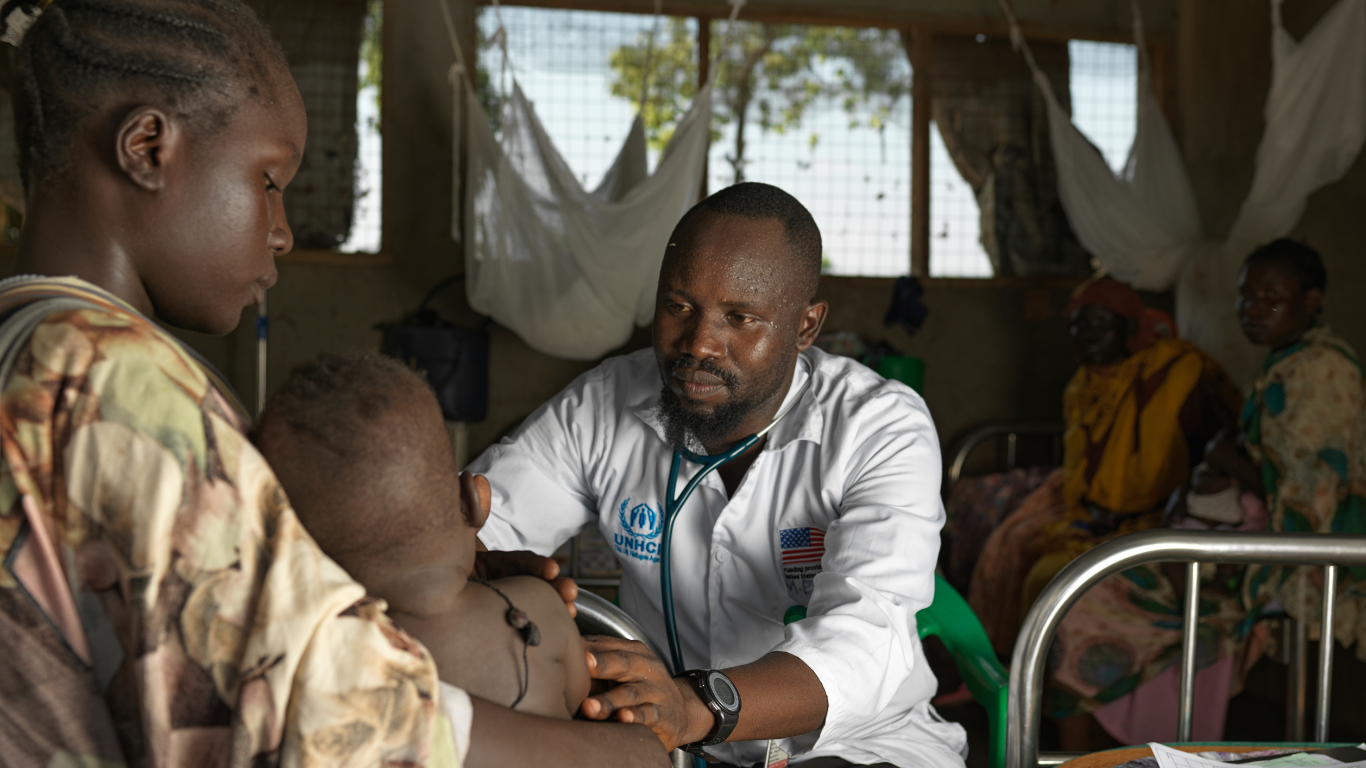
The flow of hundreds and thousands of refugees into South Sudan due to the conflict in Sudan sees most of the population struggling to access even the most basic necessities. Seven million South Sudanese face extreme hunger, rising food prices and low food production.
This situation unfolds against the backdrop of an overburdened health system, made fragile in part due to the conflict. The World Health Organization (WHO) cites inadequate infrastructure, service utilisation, and a shortage of healthcare workers as areas of concern.
Across the country, periods of drought and flooding due to climate change are creating conditions where infectious disease spreads with ease. The logistical challenges are considerable as people are cut off from medical assistance, food, supplies and their crops destroyed by floodwaters.

© Peter Caton/Relief International
Since 2006, Relief International has provided life-saving health and nutrition interventions through primary healthcare services that operate in some of South Sudan’s most challenging and disconnected communities. These services are crucial not only for the basic service provision they provide, but also because electricity, clean water and medicine can often all be found there, which brings communities to their doors.
Relief International, in partnership with United Nations High Commissioner for Refugees (UNHCR), is the sole provider of health services in Maban, a county in northeastern South Sudan, where more than 140,000 refugees reside. In addition to primary healthcare, their initiatives also include training programmes for families where a member has been diagnosed with clinical malnutrition and rehabilitating damaged water pumps to mitigate the risk of waterborne diseases. From January to December 2023, Relief International conducted over half a million curative consultations across all 11 health facilities in Maban.
With aid taking days to reach the most remote communities, and qualified medical personnel being scarce, the teams that deliver this vital care demonstrate innovation and resilience in the face of one of the biggest human displacement crises worldwide.

© Peter Caton/Relief International
“I made a decision. As long as I’m alive, I’ll find my way [to South Sudan].” – Mustafa
For many of those arriving in South Sudan, their journey has already been an ordeal. Poor health can be made worse by the weeks-long trek across borders. Mustafa, a refugee in Maban, was already severely ill and struggling to walk when he fled Sudan for South Sudan. His family thought he was joking when he told them of his plan, and unable to convince them to join him, he left alone.
In Maban, Relief International provides a lifeline for many who have endured an exhausting journey to reach South Sudan. Among the other newly arrived refugees in the camp is Abdullah Al Hamadani, a farmer who saw his crops destroyed by conflict in Sudan. His story is not unusual, with malnutrition and the loss of livelihoods a common outcome for people caught between conflict and climate change.
After a journey marked by extreme hunger, he and his family received critical care from Relief International, a first step in their long journey to recovery. Displacement has left many in South Sudan vulnerable to contracting measles, and tuberculosis (TB). These outbreaks have increased due to the compounded effects of cramped conditions, densely packed refugee settings, poor hygiene facilities, and the impacts of climate change.
Nadiri Samuel, a programme manager and medical doctor by training with Relief International, points out that malaria outbreaks are often seasonal, worsened by floods and extreme weather events. “Just a few months back, most of our health facilities were out of stock for antimalarials. Out of stock completely. Imagine coming to a health facility and you don’t have antimalarials and maybe 50% of your cases are malaria. It’s difficult.”

© Peter Caton/Relief International
“When I lost my mother, I took that initiative. I promised I’d never see any mother die in my hands.” – Poni Betty
At the heart of Relief International’s services lie the healthcare workers providing crucial care. Poni Betty’s motivation to become a midwife stems from a personal tragedy when her mother died during childbirth without a midwife available for support.
After hearing the story of Albit Leo, a refugee who was resistant and distrustful of midwives after three miscarriages, Betty took a special interest in her case and was determined that her next pregnancy would be different.
If Betty saw that Albit Leo had an antenatal appointment that she did not attend, she walked to her home to escort her. After her first successful birth, Albit Leo and her husband named her first child Betty in honour of the midwife they felt made it possible.
Betty, Cune Alice and the other midwives oversee an average of 44 births each week. They are also involved in screening and treating malaria, as rates are particularly high among pregnant women, and responded to cases of gender-based violence (GBV). They have developed an innovation so that they can prioritise cases of GBV in situations where women might not feel able to speak up.
“[Women] can pick a green leaf… hold it in their hand, so even in cases where midwives, doctors or nurses are all busy; they can see the green leaf and know this is a [GBV] emergency,” says Alice.
In Maban, at Relief International run health facilities, 96.6% of deliveries are attended by skilled health personnel, compared to the national average of 39.7%.

© Peter Caton/Relief International
“They can pick a green leaf. Any green leaf.” – Cune Alice
Resilience alone cannot deliver babies or address disease outbreaks. But the experiences of Relief International’s national staff can bring ingenuity and motivation to their work.
“My grandfather was a medical doctor, he was treating tuberculosis cases in the city,” says Mulu Esio, a clinical officer supporting refugees, and once a refugee himself, who attained his primary and secondary education in a refugee camp during the war. “He died during the fighting, he was hit by a bomb… so I felt there was unfinished business that he left.”
The international community has a vital role to play in helping to ensure these professionals have the essential supplies they need to deliver and scale up health interventions that are already working. In the face of a growing crisis and possible funding cuts, urgent global attention and support could sustain the efforts of local health professionals, like Betty, Alice, Samuel and Esio, who are going above and beyond for the communities they serve.

© Peter Caton/Relief International